Tag: thromboembolism
VTE in Critically Ill Adult Patients with Hematologic Malignancy
Among patients with hematologic malignancy, critical illness and certain baseline characteristics were associated with a higher incidence of venous thromboembolism (VTE). Among 76,803 eligible patients (mean age 67 years... read more

Handbook for Venous Thromboembolism
A truly practical guidebook for anyone who needs the key information on the diagnosis, management and prevention of venous thromboembolism. Specific areas of focus include understanding the risk factors for VTE and the role... read more
Algorithm to Predict Thromboembolism in COVID-19 Patients
Patients with COVID-19 are at increased risk for thrombosis and might be stratified on admission based on lower Pao2/FiO2 ratio, higher D-dimer levels and history of major hemorrhages. 64 thromboses were recorded in 54... read more
Risk of Serious Blood Clots Up To 6 Months After COVID-19
A study from Sweden finds an increased risk of deep vein thrombosis (a blood clot in the leg) up to three months after COVID-19 infection, pulmonary embolism (a blood clot in the lung) up to six months, and a bleeding event... read more
Sepsis Hospitalization and Risk of Subsequent Cardiovascular Events in Adults
Adult sepsis survivors experience an increased hazard of major cardiovascular events compared to survivors of a non-sepsis hospitalization. 254,241 adult sepsis survivors were matched to adult survivors of non-sepsis hospitalization... read more
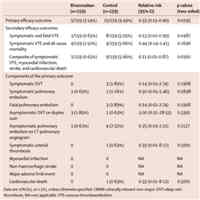
Anticoagulation Post-Discharge in Patients Hospitalized Secondary to COVID-19
This study contains interesting data that could contribute to the standard of practice when treating patients after hospitalization for COVID-19. However, use caution when applying the results of this study. Several problems... read more
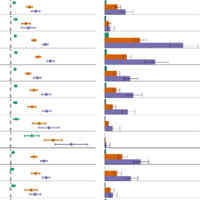
Long-term Cardiovascular Outcomes of COVID-19
The cardiovascular complications of acute coronavirus disease 2019 (COVID-19) are well described, but the post-acute cardiovascular manifestations of COVID-19 have not yet been comprehensively characterized. Here we used... read more
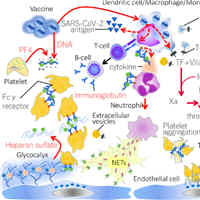
Recognizing Vaccine-Induced Immune Thrombotic Thrombocytopenia
Vaccine-induced immune thrombotic thrombocytopenia is a serious complication of vaccination that is not feasible to anticipate or prevent. When the patient presents with sustained headache, neurologic symptoms/signs,... read more
A New Risk Assessment Model for Hospital-Acquired Venous Thromboembolism in Critically Ill Children
Using the multicenter Children’s Hospital-Acquired Thrombosis registry, we identified five independent risk factors for hospital-acquired venous thromboembolism in critically ill children, deriving a new hospital-acquired... read more
Subsegmental Pulmonary Embolism Increased Rate of Recurrent VTE
Overall, patients with subsegmental pulmonary embolism who did not have proximal deep venous thrombosis had a higher-than-expected rate of recurrent venous thromboembolism (VTE). Recruitment was stopped prematurely because... read more

Optimal Follow-up After Acute Pulmonary Embolism
This position paper provides a comprehensive guide for optimal follow-up of patients with acute pulmonary embolism (PE), covering multiple relevant aspects of patient counselling. It serves as a practical guide to treating... read more
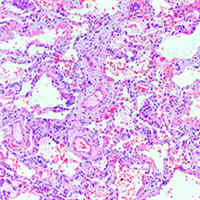
ARDS and High Blood Endocan Profile During COVID‑19
With great interest, we read the recently published paper by Pascreau et al. concluding that a high blood endocan profile during COVID‑19 distinguishes moderate from severe acute respiratory distress syndrome (ARDS). In... read more
Nitrous Oxide Avoidance for Patients Undergoing Major Surgery
Avoidance of nitrous oxide and the concomitant increase in inspired oxygen concentration decreases the incidence of complications after major surgery, but does not significantly affect the duration of hospital stay. The... read more
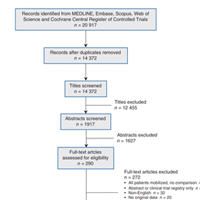
Ambulation Alone Not Effective Prophylaxis for Venous Thromboembolism
Our systematic review failed to find high-quality evidence to suggest that ambulation alone is an appropriate or effective prophylaxis for venous thromboembolism. Although some studies suggest that ambulation may reduce... read more




