Tag: ventilator

Monitoring Mechanical Ventilation Using Ventilator Waveforms
This book discusses the interpretation of mechanical ventilator waveforms. Each page shows a screenshot from a real patient and explains one or two messages. It starts with basic information about the waveforms and goes... read more

Noninvasive Mechanical Ventilation: Theory, Equipment, and Clinical Applications
The new edition presents updates regarding new clinical applications of noninvasive mechanical ventilation and discusses recent technical advances in this field. The opening sections are devoted to theory, equipment, with... read more

Mechanical Ventilation in Emergency Medicine
This book discusses mechanical ventilation in emergency settings, covering the management of patients from the time of intubation until transfer to the ICU. It provides an introduction to key concepts of physiology pertinent... read more
Pros and Cons of Disconnecting the Ventilator During Acute Respiratory Decompensation
Disconnecting the ventilator and manual BMV should be performed in cases where device malfunction is the primary cause of decompensation. These instances are quite rare. Disadvantages of switching to BMV include loss of... read more

Mechanical Ventilation for the ICU Resident: A Concept Based Approach
This book is written primarily with the intent of helping medical residents understand the basics of mechanical ventilation. It is meant to be read during a one-month rotation in the ICU. It is a compilation of concepts... read more

Clinical Application of Mechanical Ventilation
Fundamental concepts of respiratory physiology and the day-to-day duties of a respiratory care professional. Utilizing the wide degree of topics covered, including airway management, understanding ventilator waveforms,... read more
New WHO Toolkit Focuses on Severe Acute Respiratory Infection
During the early months of the pandemic, it became imperative to share best practices for the care and treatment of patients with SARS CoV-2. This new infectious agent, with potentially new pathogenesis and an unprecedented... read more
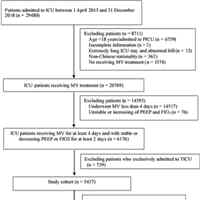
Fluid Balance and Ventilator-Associated Events Among Patients Admitted to ICUs in China
There was nonlinear relationship between fluid balance and all three tiers of ventilator-associated event, with an fluid balance between –1 and 0 L corresponding to the lowest risk. Positive but not negative fluid balance... read more
Facemask vs. Helmet – Noninvasive Ventilation
We use Noninvasive ventilation (NIV) to treat various disease processes, such as acute hypercapnic and hypoxemic respiratory failure, post-extubation failure, and neuromuscular diseases. Data supports NIV use in some conditions,... read more

Ventilator Management: A Pre-Hospital Perspective
The goal of this book is to provide the most up to date information on mechanical ventilation based on current research, evidence based practice and my experiences as a flight paramedic and educator. A comprehensive look... read more

Validation of RSBI Displayed by the Ventilator vs. Standard Technique in Patients with Readiness for Weaning
The ventilator significantly overestimates the RSBI value compared to the standard technique by Wright spirometer. The average RSBI vent value among 5 time points (0, 15, 30, 45, and 60 s) was found to best correlate with... read more

Early Tracheotomy Shortens ICU Stay and Lowers Risk of VAP
Compared with late tracheotomy, early intervention was associated with lower ventilator-associated pneumonia (VAP) rates and shorter durations of mechanical ventilation and ICU stay, but not with reduced short-term, all-cause... read more
Innovations in ICU Ventilation
Many centuries ago, Socrates stated that "the secret of change is to focus all of your energy, not on fighting the old, but on building the new." Nowadays, we may relate his quote with the concept of innovation, which is... read more
Natriuretic Peptide–driven Fluid Management during Ventilator Weaning
Our results suggest that a BNP-driven fluid management strategy decreases the duration of weaning without increasing adverse events, especially in patients with left ventricular systolic dysfunction. In a randomized controlled... read more




