Tag: ARF

Lung Ultrasound in the Critically Ill: The BLUE Protocol
Written by a pioneer in critical care ultrasound, this book discusses the basic technique and "signatures" of lung ultrasound and explains its main clinical applications. The tools and clinical uses of the BLUE protocol,... read more
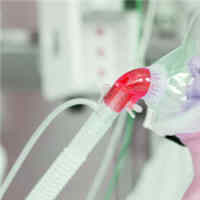
HFNO Alone or Alternating with NIV in ARF Patients
In critically ill immunocompromised patients with acute respiratory failure (ARF), the mortality rate did not differ between HFNO alone and non-invasive ventilation (NIV) alternating with high-flow nasal oxygen (HFNO). However,... read more
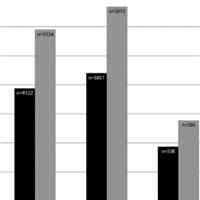
Epidemiology and Outcomes of Critically Ill Children at Risk for PARDS
The Pediatric Acute Lung Injury Consensus Conference “at-risk for pediatric acute respiratory distress syndrome” criteria identify critically ill children at high risk of pediatric acute respiratory distress syndrome... read more

Renal Failure and Replacement Therapies
Increased recognition of the overlap between critical care and renal medicine, and recent advances in the understanding of acute renal failure (ARF) and the application of renal replacement therapies (RRTs), have brought... read more

Effect of High-Flow Oxygen Therapy vs Conventional Oxygen Therapy on Invasive Mechanical Ventilation and Clinical Recovery in Patients With Severe COVID-19
An overall good trial that supports the use of high flow oxygen therapy in patients with Severe COVID-19. Randomized controlled trial conducted across three centers in Columbia over 5 months from August 2020 to January... read more

Dynamic and Hybrid Configurations for ECMO
Dynamic or hybrid configurations for extracorporeal membrane oxygenation (ECMO) are needed when patient physiology or clinical conditions change. Dynamic configurations included configurations converting from veno-arterial... read more
Bridging the Gap Between Intensivists and Primary Care Clinicians in ECMO for Respiratory Failure in Children
All pediatric clinicians should be aware not only of the potential benefits and complications of ECMO but also that survivors need effective screening, support, and follow-up. The 2009 influenza A(H1N1) pandemic, along... read more
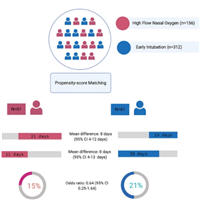
High-flow nasal oxygen in patients with COVID-19-associated acute respiratory failure
The use of high-flow nasal oxygen upon ICU admission in adult patients with COVID-19 related acute hypoxemic respiratory failure may lead to an increase in ventilator-free days and a reduction in ICU length of stay, when... read more
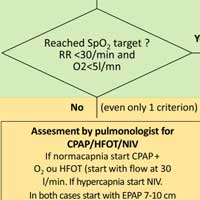
Respiratory Support in Patients with COVID-19
Non-invasive respiratory support could be useful in treating COVID-19-related acute respiratory failure (ARF). A rational use of different techniques (oxygen therapy, CPAP, NIV or HFOT) by a trained pulmonologist could allow... read more
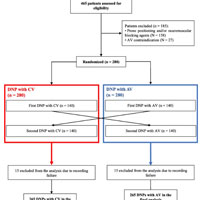
Automated vs. Conventional Ventilation in the ICU
Automated ventilation (AV) appears to reduce the incidence and severity of blood oxygen desaturation during daily nursing procedures (DNPs) in comparison to Conventional Ventilation (CV). Of the 265 included patients,... read more
Respiratory Strategies for Patients with Suspected or Proven COVID-19 Respiratory Failure
The trial objective is to determine if Continuous Positive Airway Pressure (CPAP) or High-Flow Nasal Oxygen (HFNO) is clinically effective compared to standard oxygen therapy in patients with confirmed or suspected COVID-19. The... read more
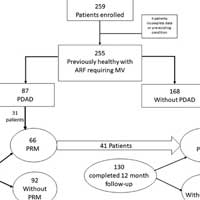
Development of Persistent Respiratory Morbidity in Previously Healthy Children After ARF
Persistent respiratory morbidity develops in up to potentially 44% of previously healthy children less than or equal to 24 months old at follow-up after acute respiratory failure (ARF) requiring mechanical ventilation. This... read more
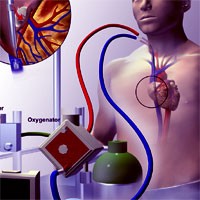
Long-Term Health-Related Quality of Life After Venovenous Extracorporeal Membrane Oxygenation
This study examined the long-term health-related quality of life in adult patients treated with venovenous extracorporeal membrane oxygenation (V-V ECMO) for severe acute respiratory failure in Ireland. A retrospective, cross-sectional... read more
Prone Positioning in Nonintubated Patients with COVID-19 and Hypoxemic Acute Respiratory Failure
In this study of patients with COVID-19 and hypoxemic respiratory failure managed outside the ICU, 63% were able to tolerate PP for more than 3 hours. However, oxygenation increased during PP in only 25% and was not sustained... read more




